College of Health
37 The Effect of Mild Traumatic Brain Injury on Turning Smoothness
Cameron B. Jensen; Paula Johnson; Nicholas Kreter; Selena Cho; Leland Dibble (Physical Therapy and Athletic Training); and Peter Fino (Health and Kinesiology)
Faculty Mentor: Peter C. Fino (Health & Kinesiology, University of Utah)
Introduction
Mild traumatic brain injuries (mTBIs; i.e. concussions) can impair a person’s motor function, and emerging research suggests that more dynamic tasks, such as turning, are particularly susceptible to the effects of mTBI [1,2.] While previous work has focused on speed and balance during turning [1,2], the smoothness of a turn may also be important; the ability to perform planned movements in a smooth, non-jerky manner is an important marker of a neurologically healthy motor control system [3]. As the effects of mTBI on the smoothness of turning remain unclear, this study sought to examine the acute and longitudinal effects of mTBI on movement smoothness during turning. We hypothesized that those with an mTBI would exhibit less smooth turns, and smoothness would improve as individuals recovered from their mTBI.
Methods
As part of a larger IRB-approved protocol, 16 healthy controls and 10 mTBI subjects provided informed written consent and walked around a turning course for 150 seconds for each condition. The two conditions were normal and fast walking. The turning course consisted of turns of varying angles. Each subject was tested at an acute time point (within 2 weeks of receiving an mTBI) and then tested again three months later. Kinematic data were recorded from inertial measurement units (IMUs, APDM Opals, Portland, OR), and smoothness of axial rotation was quantified using log dimensionless jerk from the angular velocity data in the transverse (yaw) plane, along with the average lap completion time [4]. Movements with less jerk are described as being smoother. A linear mixed model was fit for the outcome measure of smoothness with fixed effects of lap time, mTBI, time (i.e., visit), the group*time interaction, and random intercepts for each participant.
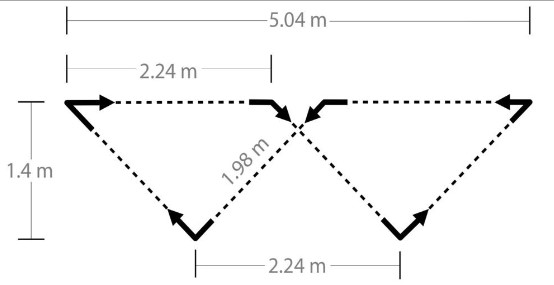
Figure 1: An IMU was worn on the lumbar region and collected kinematic data as the participant completed laps around the turning course.
Results and Discussion
A significant group*visit interaction was observed for normal speed walking when adjusting for lap time (p=0.01), where the mTBI group decreased smoothness over time relative to the controls. Faster lap times were associated with smoother axial rotations (p=0.04). A similar result was observed in the fast-walking condition as a significant decrease in smoothness was observed in the mTBI group (p=0.01), with a noteworthy but non-significant group*visit interaction (p=0.10). These results indicate that faster turning speeds are associated with more smooth turns. While mTBI subjects increased their speed over the course of recovery, their smoothness decreased, which was the opposite of the standard relationship between smoothness and speed /duration[5].
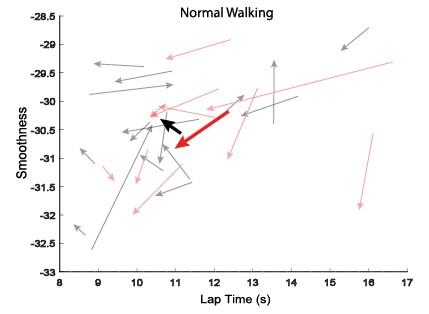
Figure 2: From the initial visit to the follow-up visit the mTBI subjects turned less smoothly while decreasing their lap time (increasing their speed). Smoothness values closer to 0 are considered more smooth.
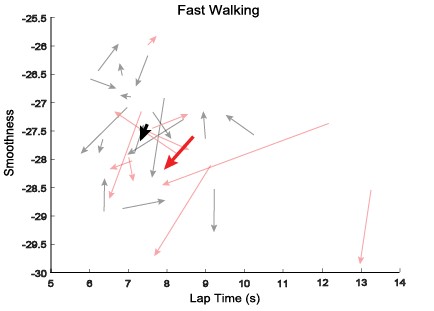
Significance
The decreased smoothness with increasing speed from the initial visit to the follow-up visit suggests that those with an mTBI are experiencing incomplete recovery and may indicate lingering issues that are not captured by turning speed alone. This causes concern for symptom provocation and injury risk. Future research will look at other factors that may impact smoothness (e.g. symptoms), and explore clinically meaningful changes in smoothness.
Acknowledgments
Funding provided by the NIH (R21HD100897 ; PI:Fino) and the University of Utah Udergraduate Research Opportunity Program (Jensen)
References
[1] Fino et al., (2018). J Neurotrauma 35(10): 1167-1177.
[2] Fino et al., (2016). J NeuroEngineering Rehabil, 13, 65.
[3] Hogan et al., (2009). J of Motor Behavior, 41:6, 529-534.
[4] Parrington et al., (2021). Gait & Posture, 90, 245-251.
[5] Balasubramanian et al., (2015). J NeuroEngineering Rehabil, 12, 112.

